Hip dysplasia that finally
gets the attention it deserves.
Hip dysplasia — also called acetabular dysplasia or DDH in adults — means the hip socket is too shallow to fully cover the ball of the hip. The result is a joint that is less stable than it should be, with more load concentrated on the labrum and cartilage.
It is the opposite of FAI — where FAI involves too much bone, dysplasia involves too little coverage. But like FAI, having the structural finding on a scan does not automatically mean surgery.
It is also one of the most commonly delayed diagnoses in young adult hip pain — particularly in women. If you have been told your hip looks normal but something still does not feel right, dysplasia is worth investigating properly.
The Diagnosis
Understanding dysplasia types
Dysplasia exists on a spectrum. The degree of undercoverage shapes both the symptoms and the management approach.
LCEA between 20 and 25 degrees. The socket is shallower than ideal but not severely so. Often manageable with conservative physiotherapy-led care.
LCEA below 20 degrees. The socket provides insufficient coverage of the femoral head. Symptoms tend to be more significant and the labrum carries more load than it should.
When the labrum has become damaged or overloaded as a result of the shallow socket. The labrum is compensating for insufficient bony coverage and can develop tears over time.
Symptoms
Do you recognise these?
Hip dysplasia in adults is often missed for years. Here is what it actually feels like.
Often described as a deep aching pain in the groin, front of the hip, or sometimes the buttock. It tends to worsen with prolonged activity or end-of-range hip movement.
A sensation that the hip is loose, giving way, or ‘slipping out.’ This is one of the more distinctive features of dysplasia — patients often describe it as their hip not feeling secure.
Running, jumping, or anything high-impact can provoke symptoms. The joint is working harder to compensate for reduced bony coverage, so load tolerance is often lower.
Many people with dysplasia notice the muscles around the hip tire quickly. This is the body recruiting extra muscular stability to compensate for what the bony architecture isn’t providing.
The labrum in a dysplastic hip is under significant stress and can become damaged. Clicking, catching, or clunking sensations can indicate labral involvement.
Hip dysplasia is one of the most commonly missed diagnoses in young adults — particularly women. Many patients spend years being told it is nothing before getting the right answer.
Setting the record straight
Hip dysplasia myths worth busting
This condition carries more misinformation than almost any other hip diagnosis. Let me be direct.
This is the most common misconception. Adult hip dysplasia is a real, significant condition. Many people have borderline or mild dysplasia that goes undetected until symptoms develop in their 20s, 30s, or later — particularly in active women.
Not necessarily. Surgery such as a periacetabular osteotomy (PAO) is an option for some, but conservative management — structured physiotherapy, load management, and strength work — can significantly improve symptoms and function for many people, particularly those with borderline presentations.
This is wrong. While the bony architecture does not change, muscles are the best brace a dysplastic hip has. A well-structured programme builds the stability the shallow socket is not fully providing — and for many people, that is enough to live and train without significant limitations.
Standard X-ray views can miss dysplasia if not specifically requested or measured. LCEA measurement, weight-bearing X-rays, and the right clinical assessment are needed. Many people are told their imaging is normal when the right measurements simply were not taken.
Treatment Approach
Building stability from the inside out
The bony architecture of a dysplastic hip does not change with physiotherapy — that is just reality. But what does change is the muscular support around it, the way the joint is loaded, and how well you can tolerate the activities that matter to you.
Muscles are the best brace a dysplastic hip has. A well-structured programme builds the hip stability that the shallow socket is not fully providing — and for many people, that is enough to live and train without significant limitations.
Understanding the degree of dysplasia, what is driving symptoms, and whether there is labral involvement. Imaging — usually X-ray first — is important here.
Understanding why the hip behaves the way it does, and learning to manage load intelligently — reducing provocation without becoming inactive.
Building hip flexor strength, glute control, and adductor load capacity. These muscles compensate for reduced bony stability and are the key to long-term resilience.
Gradually reintroducing the movements, activities and sport loads that matter to you. Confidence built on real capacity, not avoidance.
Understanding your hip, knowing what keeps it happy, and having the tools to manage it yourself — including knowing when to seek further input.
Learn From Me
Watch: Hip dysplasia explained
Evidence-based, jargon-light. Everything you need to understand your hip.
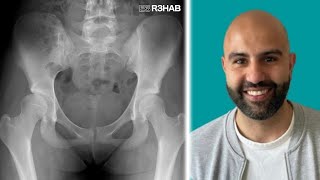
Diagnosis, the ALPHA mnemonic, when to consider imaging, management strategies and common misconceptions.
In-depth discussion on hip pathologies including dysplasia, structured loading programmes and assessment.

Is pelvic tilt actually causing your pain? What the evidence says about common misconceptions.
Online Programme
Structured rehab, built for your hip.
A dedicated hip dysplasia rehab programme — designed by me to help you build the muscular stability your hip needs and get back to doing the things you love, with confidence.
Self-Directed
Expert-designed, condition-specific rehab you follow at home. Phase-based, progressive, and built around the unique demands of a dysplastic hip.
Common Questions
Questions I get all the time
Ready to get a proper assessment?
Book an appointment in Exeter, Harley Street, or online. Let’s get clarity on what’s going on and build a plan.
Book an Appointment